
What is Andropause?
Andropause is often considered the male version of menopause and in some respects that's accurate. More specifically, both are age-related primary hormone declines, which if untreated can result in a variety of adverse symptoms. Andropause is the popular term for the condition associated with the physical and emotional changes men experience as they age, but it goes by several aliases including late onset hypogonadism, androgen decline in the aging male (ADAM), and male climacteric andropause. Although traditionally attributed to aging, many of the negative effects men start to experience as they get older are caused by a significant decrease in testosterone (the primary male hormone) production, which results in diminished hormone levels.
The primary difference between menopause and andropause is that of speed. Whereas menopause is a rather sudden, succinct and more defined change andropause isn't. Its onset, and declining testosterone production, begins around age 30 and progresses (at a rate of approximately one percent per year). Researchers estimate the incidences of andropause in our society as follows: ages 40 to 49 at least 2% to 5% of men could be clinically diagnosed with the condition; ages 50 to 59 anywhere from 6% to 30%; ages 60 to 69 between 20% and 45%; ages 70 to 79 from 34% to 70% and; 80 plus at nearly 91%. These numbers unfortunately in reality are probably much higher in todays society.
What Testosterone Does
Of course testosterone is present in both males and females; however, males produce approximately ten times more testosterone than their estrogen-based female counterparts. Testosterone is the male body's primary natural hormone, and is integral to male development from birth onward with responsibilities which include: determining gender, moderating pubertal changes; maintaining male potency (libido & sexual functioning) and; the partitioning of bodily muscle and fat distribution. It is also a foundational to a male's sense of well-being, and figures prominently in physiological, biological, and sexual health, while influencing sperm production, stress coping capacity, mental acuity (clarity, memory & recall, concentration & focus), bone density, red blood cell production, and immune system support. So it's easy to see why so many elements of health begin to breakdown as andropause progresses.
Symptoms of Andropause
The symptoms of andropause syndrome are the same as those of non-age related testosterone deficiency, a.k.a. low testosterone, and are characterized by:
- Low hemoglobin/hematocrit and possibly mild anemia
- Lower energy levels, and reduced interest in usual activities
- Increase in fat between and surrounding internal organs (visceral)
- Loss of bone density which increases the risk of osteoporosis, fractures, and breaks
- Declining strength, and reduced lean body mass
- Atypical cholesterol and lipid values
- Loss of hair (thickness and/or amount)
- Mood swings, irritability, depression, anger and fatigue
- Loss of sexual desire and erectile dysfunction
Testing for Andropause
Physicians use a simple blood test to measure testosterone levels including bound (that which is attached to Sex Hormone Binding Globulin - SHBG), and 'free' (unbound). Typically Testosterone deficiency is diagnosed when testing returns a total testosterone serum level is below 350 ng/dl. An educated physician knows how to accurately and correctly diagnose for low testosterone. First listening to the patients symptoms and a proper health history is taken into account first and foremost; then labs correctly interpreted by a skillfull physician. The most important lab value is not the total testosterone level at all. It's the free testosterone is what's important here. Free testosterone is the unbound therefore "free" to circulate in the body building muscles, bones and giving us our mojo. Only makes since that this is the level to watch. Free testosterone only makes up 1-2% of total testosterone because the other 98% is bound up and occupied by proteins. Most men will start experiencing symptoms of declining testosterone when their free testosterone reaches 150 pg/dl or 15 pg/ml and symptoms intensify as levels continue to decline. The blood test should administered in the morning, prior to daily stressors which can influence testosterone production such as work, exercise, medication, etc.
Men who are of age, and complain about symptoms directly related to andropause, may also require measurements and evaluations of LH (luteining hormone) and FSH (follicle stimulating hormone).
Testosterone Replacement Therapy
Prescribed testosterone preparations, along with their prescribed dosages and frequency of treatment are customized into what is collectively known as hormone replacement therapy (HRT), or as testosterone replacement therapy (TRT).
TRT is a highly effective treatment program for andropause, and numerous additional causes of low testosterone production, but it's not the only remedy. There are times when certain pituitary problems require non-hormonal medication, radiation treatments, surgical removal of a pituitary tumor, or the replacement of other bodily hormones.
Testosterone Preparations
There are a multiple testosterone preparations to choose from, and several reasons to select one over another. Each of the following choices will provide adequate hormone replacement, along with inherent pros and cons. The trick is to find the one that fits you best.
Oral tablets are great, and their vitamin-like convenience and ease of use make them especially popular. Lots of men prefer this method because they're already accustomed to taking vitamins, and are usually uncomfortable with needles. However, tablets are harsher on the liver, and generally require daily or twice daily to administration to sustain blood serum levels. Some Patients also experience a roller coaster effect as there levels can yaw up and down with this treatment method. Probably the biggest obstacle to tablet taking is forgetfulness. Some men simply can't remember to routinely take their meds, and thus would be better off with a method that's less frequent.
The testosterone patch comes in a variety of dosages and brands, among which are the very popular Androderm and Testoderm. The patch requires daily changing, and some users find it uncomfortable, while experience allergic reactions in the form of skin irritations to its adhesive. Also some patients only get a mild bump in there levels or none at all after awhile and require a more effective delivery method. Nevertheless, the testosterone patch is still a efficient and popularly used testosterone delivery mechanism. Earlier models of the patch required attachment to the scrotum and genitals, but today's patches can be applied to clean, dry areas on the thighs, back, stomach, or upper arms. Consistency is also an issue, as you'll have to rotate sites daily, allowing at least 7 days before reusing a site.
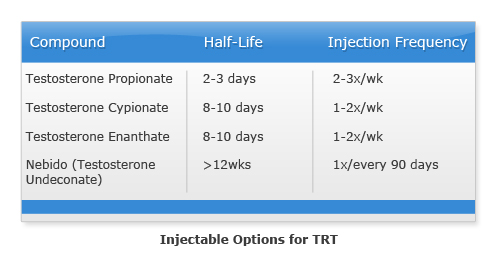
Even the word 'injectable' strikes fear in the hearts of some, yet injectables are the single most frequently used form of TRT. Testosterone injections are shot directly into the muscle, and then absorbed into the bloodstream via the capillaries. Intramuscular (IM) testosterone injections are not only popular because of their differing time release options, but also because they don't disrupt liver functioning. IMs have esters have added to the preparation to control its speed of release and consequently, its rate of activity within the body. The U.S. has approved four primary TRT preparations:
Another daily administered preparation, the testosterone gel, combines the qualities of several applications. For example, it shares transdermal (through the skin) absorption with the patch, requires daily administration like both the patch and tablets, and elevates serum levels quickly like both the aforementioned mechanisms as well as intramuscular testosterone propionate. Mostly due to its great convenience, testosterone gel has been a very popular preparation since its debut. However, again some patients only get a mild bump in there levels or none at all after awhile and require a more effective delivery method.
Lastly, long-acting Testopel is a subcutaneous crystalline testosterone pellet manufactured by Organon. This preparation has been approved in the U.S. for the treatment of testosterone deficiency syndrome in men. The Testopel pellet is inserted subcutaneously (between skin layers), and provides a sustained testosterone release for 3-6 months. Although these pellets are just as effective as the other preparations cited here, they are not as popular. Patients are required to undergo a surgical procedure to implant the pellets and the sensation of the pellets to some are annoying and bothersome.
Living With Andropause
So as you can see living with andropause isn't downhill spiral that it used be. Now that scientist better understand the syndrome, and physicians are equipped with the tools to combat its aversive symptoms, your golden years can be a lot more enjoyable. TRT has transformed a traditionally dreaded phase of life into one of verve, virility, and continued activeness.
